Major advances in wireless technology, miniaturization, and computing power are fueling an exponential increase in the pace and scale with which digital health care innovations are emerging and impacting both clinical and business operations. These advances are also driving an increase in the expectations of consumers that “going digital” is not enough—“being digital” appears to be the new necessity for all health care organizations – Deloitte’s Report “2019 Global Health Care Outlook” strengthens the power of digitalization.
The adage, “What goes up, must come down,” isn’t likely to apply to the global health care sector in 2019. Aging and growing populations, greater prevalence of chronic diseases, exponential advances in innovative, but costly, digital technologies – these and other developments continue to increase health care demand and expenditures. Health care stakeholders – providers, governments, payers, consumers, and other companies/organizations – struggling to manage clinical, operational, and financial challenges envision a future in which new business and care delivery models, aided by digital technologies, may help to solve today’s problems and to build a sustainable foundation for affordable, accessible, high-quality health care. This vision may have a greater probability of becoming a reality if all stakeholders actively participate in shaping the future— by way of shifting focus away from a system of sick care in which we treat patients after they fall ill, to one of health care which supports well-being, prevention, and early intervention.
This 2019 outlook reviews the current state of the global health care sector and explores trends and issues impacting health care providers, governments, payers, patients, and other stakeholders. It also outlines suggestions for them as they seek to redefine the health care ecosystem and looks at examples from the market.
Global health care sector issues in 2019
Creating financial sustainability in an uncertain health economy
Global health care expenditures are expected to continue to rise as spending is projected to increase at an annual rate of 5.4 percent between 2017-2022, from USD $7.724 trillion to USD $10.059 trillion. The emergence of personalized medicine, increased use of exponential technologies, entry of disruptive and non-traditional competitors, the demand for expanded care delivery sites, and revamped payment and public funding models are all impacting the financial performance of the health care ecosystem. The health care market is looking to health technology for help, along with mergers, acquisitions, and partnerships.
Using new care delivery models to improve access and affordability
Moving from volume to value will require building an outcomes-based financial model and data infrastructure to maximize value-based care (VBC) reimbursement pathways, which will likely be fundamental to many health systems’ sustainable growth. This shift is the most apparent in the United States, where the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) provisions will see payment adjustments and incentive payments take effect in 2019. Clinical innovations, patient preferences, and government program payment policies are prompting hospitals to shift certain services to alternative points of care and even to virtual environments that benefit from a cost and access perspective. It is also being seen that social determinants of health often have a greater impact on health outcomes than does health care.
Adapting to changing consumer needs, demands, and expectations
Patients and caregivers, dissatisfied with poor service and lack of transparency around price, quality, and safety, are expecting health care solutions that are coordinated, convenient, customized, and accessible. With health care becoming “shoppable” and increased costs for patients in a cost sharing model, enhancing the patient experience is a potential area for dramatic change. Non-traditional companies from consumer, retail, and technology sectors are also making forays into the health care value chain with solutions that are disrupting the norm. As preventative health takes a greater role, “nudging’ is increasingly seen as an option to help with patient adherence.
Investing in digital innovation and transformation
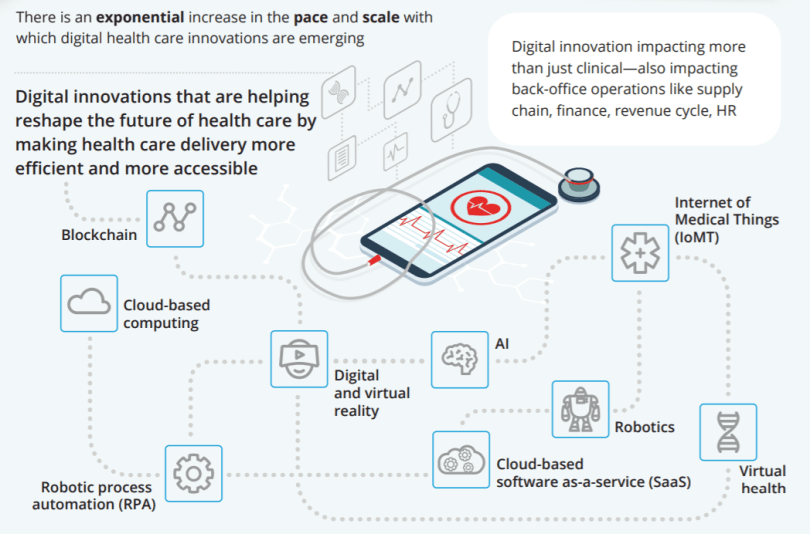
There is an exponential increase in the pace and scale with which digital health care innovations are emerging. Digital technologies are supporting health systems’ efforts to transition to new models of patient-centered care and helping them develop “smart health” approaches to increase access and affordability, improve quality, and lower costs. From Blockchain, RPA, cloud, artificial intelligence (AI), and robotics, to internet of medical things (IoMT), digital and virtual reality are just some of the ways technology is disrupting health care. These technologies are helping with diagnosis and treatment, helping with speed, quality and accuracy, and improving the patient experience.
Maintaining regulatory compliance and cyber security
As data is becoming the new health care currency, protecting it will be key. Clinical innovations, connected medical devices, and market complexity have amplified the continued need for evolving government policies, regulatory oversight, and risk management. The rapid growth of “consumptive” health services such as prescription drug pricing in the United States have recently received a lot of regulatory attention. Cybersecurity is another top concern to the industry. It is the huge volume of high-value data and growing demand for interconnected IT environments that make health care an attractive target for cybercrime.
Recruiting, developing and retaining top talent
An aging workforce, rising demand for health care services, moral and well-being concerns are driving shortages of appropriately skilled health care staff in both developed and developing economies. But, there are different dimensions shaping the future of work. While automation is impacting a number of administrative processes, telehealth and digital medicine tools are enabling a “care anywhere” model. Organizations are building and deploying new staffing models, such as allowing nurses to work remotely, while still building strong patient relationships.
Click here to download the full report.
Source: Deloitte