
The need for a paradigm shift from sick to preventive care is evident. Still, healthcare systems are mostly oriented towards medicines and hospital care while expenditure on prevention is marginal. The Nordic Health 2030 Movement wants to rearrange the existing health model. How? By changing the allocation of healthcare spending, establishing new data and business models, activating individuals. Interview with Bogi Eliasen, Director of Health at the Copenhagen Institute For Futures Studies.
What is Nordic Health 2030?
Nordic Health 2030 began in 2019 as a scenario process with over thirty leading Nordic healthcare experts from the public and private sector. We started with the workshop series to find out how to best shape the future of health in the Nordics through the lens of Agenda 2030. One of the conclusions was creating the Nordic Health 2030 movement, which strives to facilitate a shared agenda and dialogue between the ongoing efforts and stakeholders active in the health value chain.
The movement rests on three principles: The New Social Contract, The New Data Models, and The New Business Models…
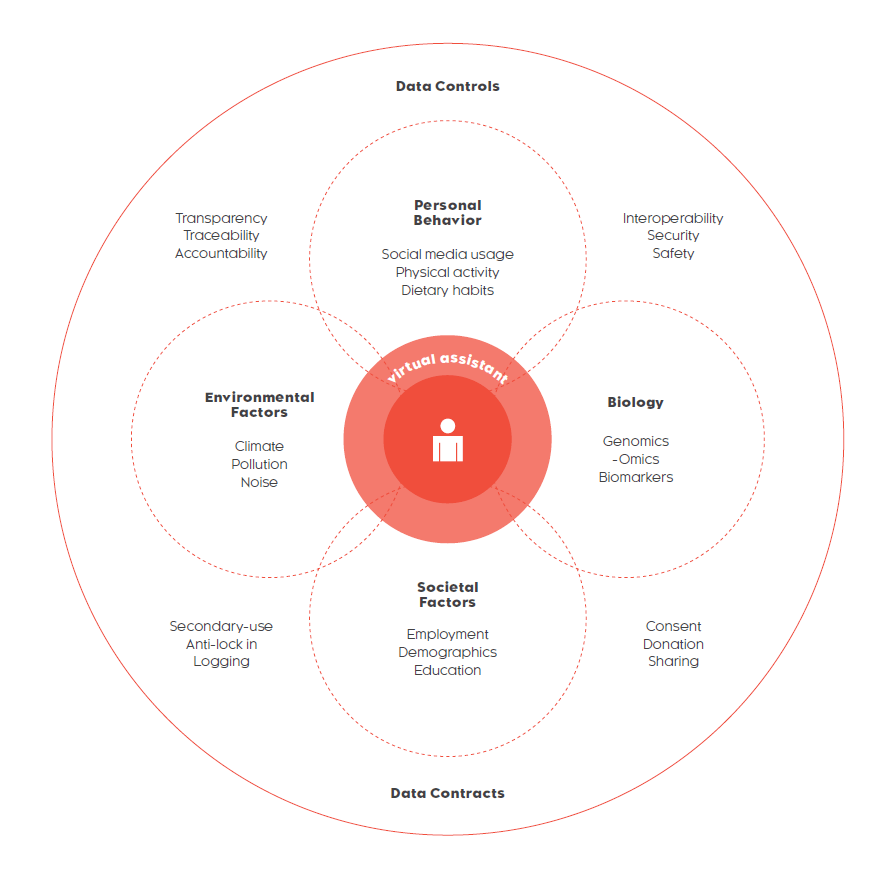
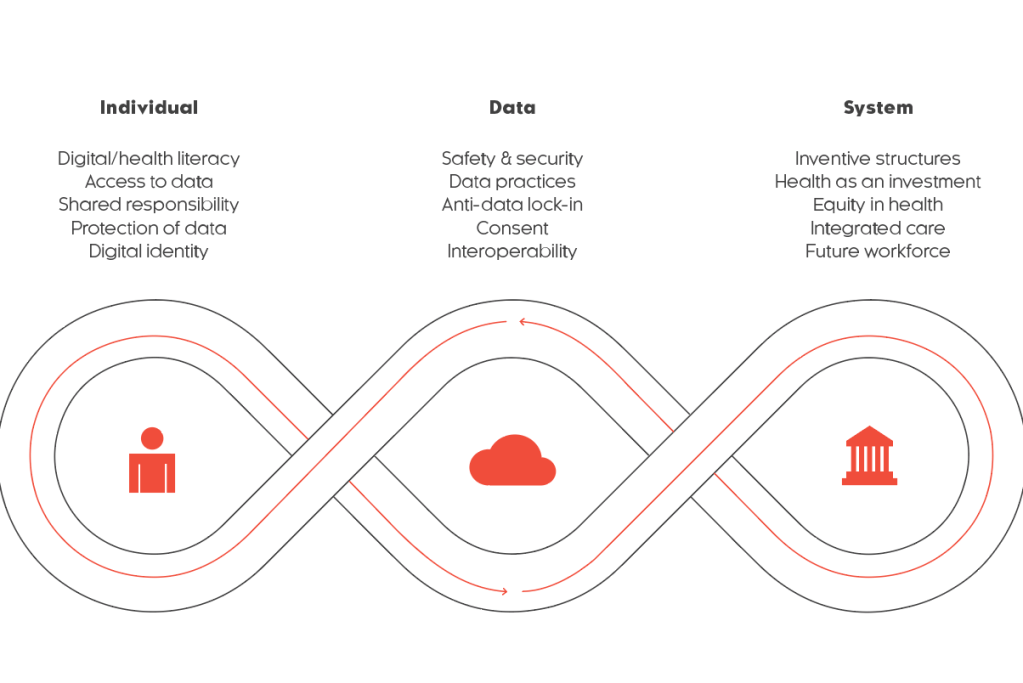
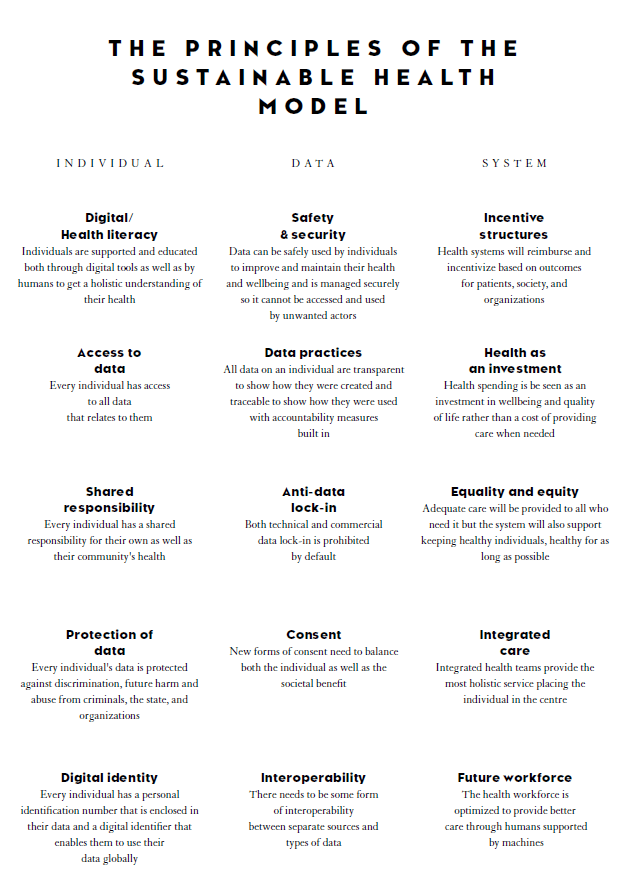
The new social contract essentially states that individuals in the future will need to be more responsible for their own health. It features six concepts related to how the individuals can take more control over their own health. The new business model states that the systems need to shift to providing preventive services while still providing treatment to individuals and equipping them with the tools required to enable them to take responsibility for their health.
Incentive structures also need to be redesigned to support organizations that provide preventive services. Data ties the individual and the system together as, without data, there is no such thing as personalized health. New data models can give individuals a better overview of their own health data, motivating them to take responsibility for their health. The system must, in return, provide the individual with tools to be able to collect and make sense of their own data.
The need for moving away from acute care to preventive health was recognized years ago. Still, this transformation faces many obstacles: existing health facilities infrastructure, reimbursement policies, culture. Finally, COVID-19 pandemic made us realize that we need hospitals to respond to unexpected health threats. How should this shift be done to succeed?
First of all, the Nordic Health 2030 philosophy does not say there is no need for hospitals – there will be still sick people in the future. We must cater to both the needs of the sick while at the same time, strive to keep healthy people healthy. Therefore, what we say is if we can prevent people from having to go to the hospital in the first place. Why would we not do that?
Regarding obstacles, I agree that the shift to prevention has been recognized long ago. In fact, in Ancient China, the doctors were only paid for the days their patients were healthy, for instance. The key difference we have today – that was not the case in the past – is access to better medical technologies and, more importantly – data. A massive amount of data provides a much better picture of an individual as well as population health. Therefore, it enables the shift from one-size-fits-all treatment to evidence-based care for everyone.
Nordic Health 2030 recognizes the power of the secondary use of data. For example, for scientific or population health purposes. How to find a balance between privacy and data safety, citizens’ trust and ethical use of data by private and public entities?
I sincerely believe ethical discussions are pockets of time and change as we make progress. Ethical discussions today are very different from the past when, for example, in vitro fertilization was completely unaccepted, at least in Denmark. Today, however, people from across the globe travel to Denmark to get treatment. Regarding the secondary use of data, I think a dynamic consent approach is the most likely balance. By implementing dynamic consent, people can choose to review and withdraw their consent at any time on a digital interface. Researchers can ask follow-up questions, ask for permission to use the already acquired data for something else, and engage the trial participants in the research.
Following the concept, by 2030, Nordic countries should allocate 5% of the GDP to treatment and 5% of the GDP to prevention. Does it mean reducing the budget for hospitals or reimbursement of medicines?
I would put it another way. It is not taking money away from hospitals and reimbursements for medicines. It is about freeing up budgets to focus more on prevention to reduce costs in the hospitals. The 5/5 aspiration is meant as inspiration to begin making the shift gradually, i.e., not closing hospitals and completely rehauling healthcare budgets but rather beginning to think more in terms of preventive measures to implement. For instance, looking at the determinants of health, we know that medical care only accounts for a fraction of individuals’ health, while behavior accounts for about one-third. Invest more in things that provide better health outcomes while also continuing to invest in cutting-edge research of disease is the key. In addition to that thought, the prevention includes promotion and primary, secondary, and tertiary prevention, so the hospital is still very much a part of it.
What is the roadmap to achieve the goals of the Nordic Health 2030 vision?
The Nordic Health 2030 Movement built up a consortium of stakeholders continually pushing towards reaching the vision. This is done through applications for grants, dissemination of knowledge, especially at the decision-maker level, and most importantly, educating and convincing people that something must be done, and soon.

I have a small favour to ask…
This content is free of charge. This website is free of commercials. Please support aboutDigitalHealth.com (€1+). It only takes a minute. Thank you!
€1.00