
2020 is the year of the COVID-19 pandemic . We have experienced the fragility of overloaded healthcare systems. We’ve celebrated doctors’ and nurses’ heroic work and realized that respirators without medical professionals do not help patients. Telecare is now regular care. Tracking apps have been installed on millions of smartphones. And what does it all means for the digitalization of healthcare?
Telemedicine
Prior to COVID-19, telemedicine was a second-class medicine, often overlooked by politicians, public health authorities, health insurers. Even though the overall share of teleconsultations was gradually increasing, their deployment was mostly driven by industry.
The pandemic changed it rapidly – virtual appointments dominated outpatient medical care. In the USA, there was a 154% increase in telehealth visits during the last week of March 2020, compared with the same period in 2019. According to the ZI Trend Report, 1.239.734 minutes of video consultation were conducted between March 4 and June 30 in Germany. It is 2126 times more than in the same period last year! Any gain by several thousand percent in a short time has its consequences. In many cases, IT solutions were implemented in a hurry with only one goal: to ensure the continuity of health services delivery.
Let’s be honest: it is impossible to smoothly switch to a new model of virtual health care overnight. What was lacking were standards and knowledge related to how to undertake care remotely, talk to the patients via computer or telephone, and support them in their illness, despite the lack of physical presence. This is much harder than just sending an electronic prescription.
Other shortcomings were in the provision of legal solutions that would guarantee fair conditions for reimbursing teleconsultations and making investments in telehealth technologies. We are dealing now with “medicine over the phone or Internet,” not “telemedicine,” whose capabilities are much more significant.
The latest report by HIMSS, “eHealth Trendbarometer on Telehealth Adoption prior to COVID-19“, clearly shows that before the pandemic outbreak, the majority of European health care providers had the right infrastructure ready. Still, telehealth solutions were rarely used in outpatient health care. Is COVID-19 alarming enough to reform inefficient health care systems, including through the use of technology?
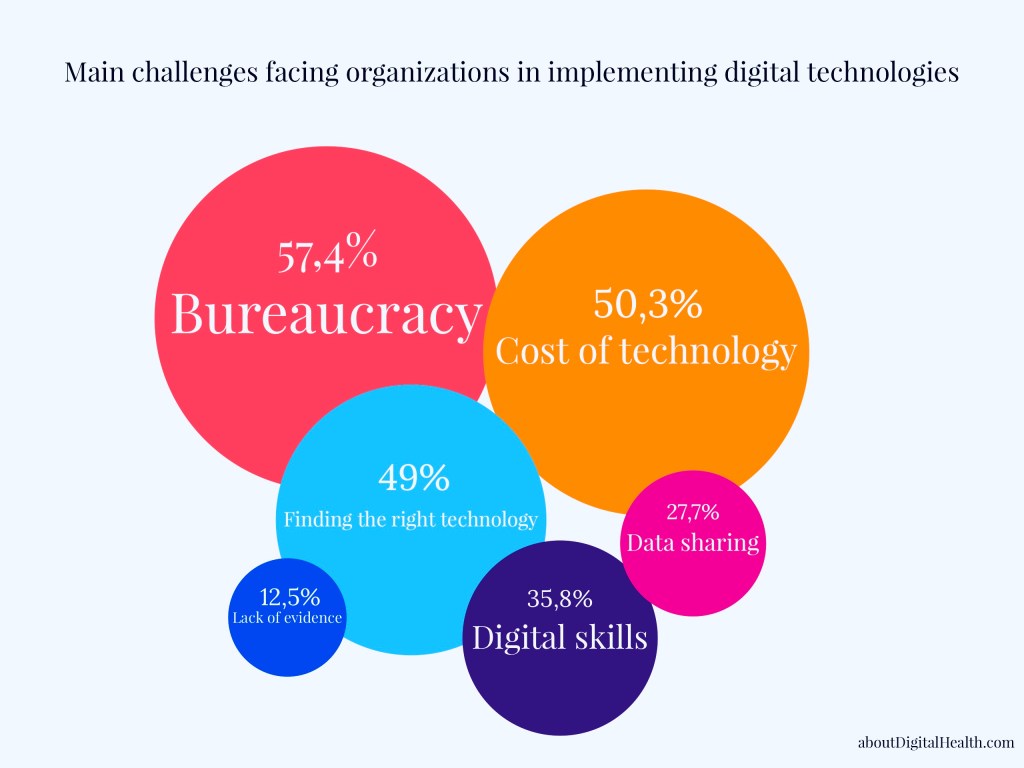
Mobile applications
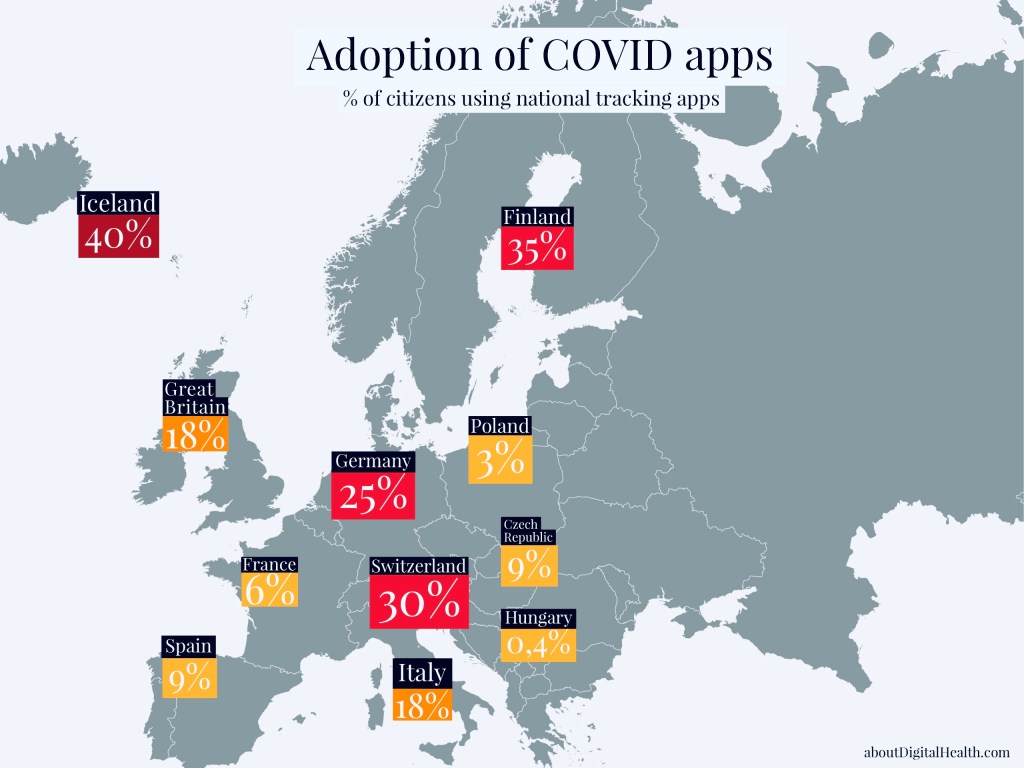
In order to control and overcome the coronavirus infections chain, many countries decided to introduce tracking applications. By the end of September, an app created by the NHS had been downloaded in Great Britain more than 12 million times (in a population of 66 million). A similar app was introduced in Germany (Corona-Warn App) and downloaded by 21 million people (in a population of 83 million). In Iceland, the COVID-19 mobile app was installed by 40% of the citizens shortly after it was launched. In Switzerland, the SwissCovid application was downloaded over 2 million times (in a population of 8.9 million). A failure in tracking app adoption was seen in France (2.4 million downloads in the middle of September in a population of 69 million), Portugal, and Poland (1,2 million downloads by the beginning of October in a population of 38 million).
The tracking app’s implementation often failed, mainly due to data safety issues (Portugal) or a low level of trust towards public authorities. We have learned that innovations are not just about the technology, regardless of the fantastic possibilities it offers. What is essential is trust, privacy, and the relevant adoption of digital solutions to the citizens’ needs and ecosystem’s specifics. No, it’s not about the right marketing and promotion. Many countries have launched COVID apps to show that they use new technologies rather than use them for health-related goals. They were convinced that the threat posed by the pandemic was reason enough to install a given solution on a smartphone. They lacked knowledge of how to introduce this type of digital health intervention on a mass scale. They lacked leadership.
Electronic health records
During the COVID-19 pandemic, it turned out that electronic health records in their current form are a bottleneck in healthcare instead of a reliable and accessible source of information about the patient.
In the hospitals, as the beds in intensive care units quickly filled up, no doctor or nurse could afford to spend extra time entering data in the EHR. Not all doctors seeing patients virtually had access to telehealth systems that offered the technical possibilities to ensure integration with existing electronic health records. They also lacked sufficient time.
According to research published in the Annals of Internal Medicine, doctors devote an average of 16 minutes and 14 seconds to handling electronic health records during an appointment with a patient. Electronic health records in their current form are ineffective. Doctors complain about the burden of administrative work and the lack of time for direct communication with patients. And they have a right to be dissatisfied.
After the pandemic, we may find that 2020 was the year when the quality of data in the patients’ health records deteriorated. We need to quickly introduce solutions facilitating the capturing and recording of medical data. This also means shifting the center of gravity of responsibility. Some information can be gathered and entered by the patient. We already today generate a lot of data ourselves. We wear smartwatches and smart bands when doing sport, measure temperature and blood pressure using older devices, or observe and record the symptoms manually manifested by our bodies. Health records need to be available to the patient, easy to use, enabling automatic data sorting, and suggesting data trends to improve the care process rather than increase the time spent looking at the screen.
Infrastructure
Implementations of new digital solutions have had to be postponed due to epidemiological restrictions. Many software and hardware investments in hospitals have been delayed. What’s obvious, all human resources in healthcare focused on patients, not on IT systems. Over 240 000 deaths have been directly attributed to COVID-19 in the USA; 1 260 000 in Europe (as for 10th of November). International Monetary Fund estimates the global pandemic cost at $28tn in lost output.
In many countries, hospitals’ financial situation has significantly worsened, and it will take months or even years until it recovers. Overstretched hospital budgets, especially in the smaller facilities, cannot sustain essential investments in hardware and software. Due to the economic crisis, public spending in IT is expected to be reduced in developing countries.
Do you know this joke? Someone asks: what has accelerated the digitalization in your organization? The answer is not CIO, neither CEO, not even CTO but COVID. Well, it’s not the case in some hospitals.

Access to digital services
When the pandemic broke out, it was feared that only digitally literate people will benefit: high educated citizens with access to technologies (computers, smartphones) and high-speed internet. At the same time, digitally excluded seniors or people with low income/education would become marginalized groups. These concerns became a reality, although not as a result of the COVID-19 pandemic. The gaps had existed before.
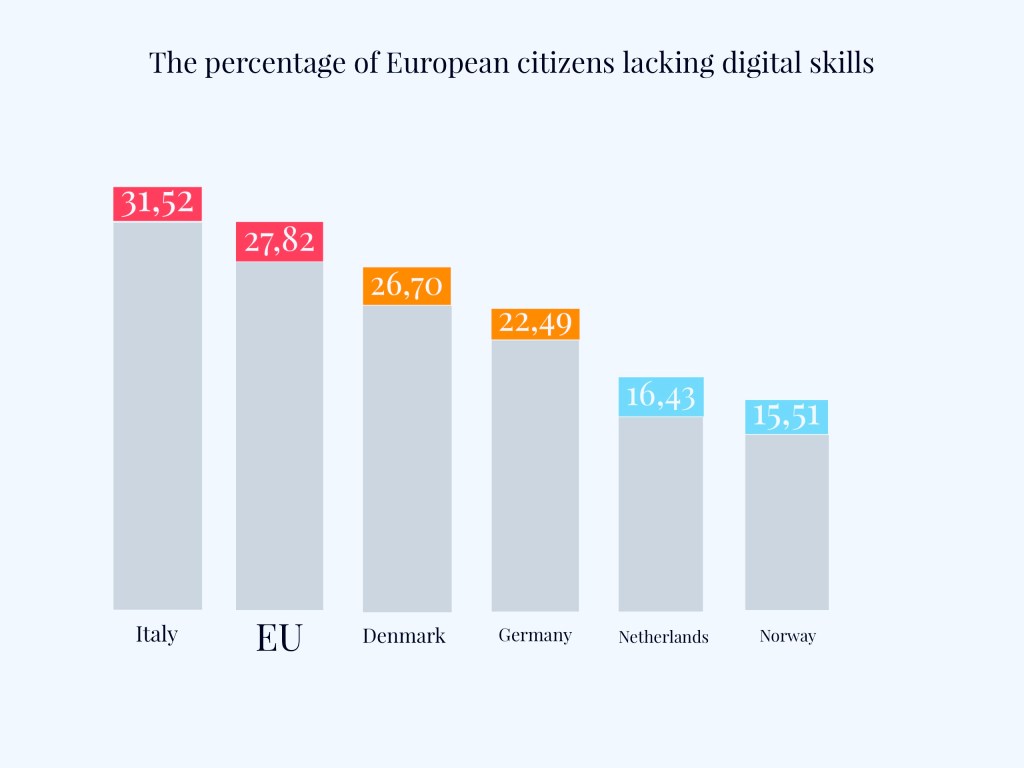
The inequalities are huge when we take into account age groups and geographical factors. While in countries like the Netherlands, Sweden, Denmark, Finland, Estonia, and Germany, over 90% of the population has access to the Internet, in less wealthy Bulgaria this percentage is 75%. In Slovakia, Hungary or Portugal it is about 80%.
According to data published by Eurostat, 94% of people aged 16-24 regularly use the Internet. This is more than twice as much as the 55-74 age group (46%). When we compare people with higher education and those with primary education, the gap is similar: 93% versus 48%. This data was collected before the COVID-19 pandemic. We can assume that the knowledge and acceptance of digital health solutions have increased, although mainly in the groups where they were already high.
The technology that saved many people from being left behind is an ordinary phone. Not a smartphone. The call, not a video-call, was the most frequently chosen by older people. Is it not a little sad that while some people can play games on their smartphones using superfast 5G Internet, others have to call their doctors or take a bus for several kilometers to get a prescription for the medications they need? I find it concerning.
Startups
Digitization in healthcare is mainly driven by startups that launch new wearables, health apps and AI-based systems. Their activity in the market depends on venture capital (VC) funds, which reflect the mood on the financial markets. Hence during the financial crisis, VC investors used to avoid risk, as associated with investing in young companies.
In March and April, everything seemed to suggest that it would be the worst year for startups. But according to the latest reports, 2020 will go down in history as the year with the highest funding for digital health startups. In 2019, funding for all transactions regarding US-based digital health startups was USD 7.4 billion, following Rock Health. By the third quarter of 2020, it has already exceeded USD 9.4 billion, and forecasts estimate about USD 12 billion by the end of the year. Asia saw a nearly triple funding increase in Q3 2020. 2020 will be the largest funding year ever for digital health.
Who has lost and who has gained? The winners may turn out to be startups working on solutions that address the pandemic’s challenges, such as telecare platforms, remote patient monitoring solutions, mental health. The companies in trouble are mostly small startups that have just started looking for their first funding and have recently started their first steps as entrepreneurs. Cancelled events limit their networking opportunities with VCs, whereas hospitals have practically suspended partnerships to develop new services or products during the COVID-19 outbreak. According to a recent survey carried out by LocalGlobe and Dealroom, 40% of European startups expect 25% revenue decrease in 2020, compared to previous targets. Over 40% of imminent fundraises have been delayed. More likely to apply for state aid are seed-stage companies. Conclusion: the big ones got bigger; the small ones might face some troubles. But the market is apparently doing well and there are many indications that it will continue to grow in 2021 (much higher economic growth after the crisis in 2020, COVID-19 effect on health care innovations).

Pharma
There is hope for 2021 since Pfizer and BioNTech announced vaccine against COVID-19 that indicates an efficacy rate above 90%. Will 2021 be the year of celebrating biotechnology advancements?
What are your thoughts?
Share your experience – click here to join the discussion on LinkedIn.

Did you like the article? Please donate
This content is free of charge. This website is free of commercials. Please support aboutDigitalHealth.com (€1+). It only takes a minute. Thank you!
€1.00
This is interesting. How about telegenetics, https://fdna.health/, AI tools for screening and diagnosis? They really connect more people than might have access before to crucial care and diagnostic tools.
LikeLike