
Doctors have been promised less paperwork and more time for the patients. Hospitals should be already packed with AI-supported systems that choose the best therapy options and support decision-making. Patients were to become empowered and healthcare – democratized. These visions have been repeated over and over again for decades.
Thirty-three years ago, in 1988, Apple published a vision of healthcare in 2008 where artificial intelligence would support clinical decision-making. Hospitals would look like 5-star hotels. All citizens would have their health monitored 24/7 to prevent diseases instead of curing them.
Another vision, presented by Microsoft 9 years ago, featured care managers looking after patients from behind the desk, with homes being transformed into health management centers. To make these promises real, we needed only digital tools: apps, wearables, smartwatches, AI-driven hospital information systems (HIS), smart electronic medical records (EDM). In the ’70s and ’80s, technology appeared to be a simple panacea.

Although a lot has changed since then, computers haven’t solved healthcare’s biggest problems. Hospitals have implemented IT systems, which certainly help them in workflow management, reporting, and patient data archiving, but they haven’t revolutionized patient care quality.
Small but crucial factors – data interoperability, digital infrastructure, reimbursement policies, data security, and the transition from an analogue to digital culture – have stood in the way of success. Why? Because this transformation is about an entirely new healthcare economy, not about putting a digital layer on top of what we have now.
Almost none of the predictions came true.
Myth #1. More time for patients
Software automatizes many processes that should reduce administrative burden, giving doctors more time for patients. However, this cause-and-effect relationship may not occur. One of the barriers is the rebound effect. You know it probably from energy-saving light bulbs. They consume less energy, so consumers tend to leave the light on for longer – if the light bulb saves energy, they don’t have to. At the end of the day, there are no savings at all.
So let’s say that the doctors save time and can see now more patients within an hour. They will probably have to see more patients because there are massive shortages of doctors. The time gained thanks to digitization does not return to the patient or the doctor, as many would wish to, but pushes the doctor to see more patients.
In digitized healthcare, the rebound effect can be twofold. Firstly, it is difficult to expect that doctors will gain more time for their patients considering that the time for an appointment is regulated, among others, by the payer, following economic calculations and waiting times or demand. If the doctor can see more patients in an hour, he or she will have to probably. The time regained thanks to digitization does not return to the patient, as many would wish.
Secondly, along with reduced waiting times due to greater efficiency and more convenient forms of medical services, such as teleconsultation, patients have the impression of better accessibility. Consequently, they use online consultation more often. It only takes a few clicks to connect with a doctor. Some studies suggest that a telehealth visit costs on average about 50 percent less compared with an office visit. But virtual visits generate additional medical use.
Moreover, a recently published study by doctors from the Mayo Clinic also gives food for thought, suggesting that the atrial fibrillation detection feature in Apple watches generates a large proportion of false-positive results, leading to unnecessary doctor’s visits of concerned patients. Paradoxically, technology increases the demand for medical services.
Myth #2. The closer to the patient, the better
With the adoption of digital technologies and AI solutions, the proportion between the time for paperwork and communication with the patient will change positively. A study based on a nationally representative survey of 4,720 U.S. physicians shows that statistically, doctors spend 16.6% of their time on administration. Assuming a visit lasts 12 minutes, that’s 2 minutes. This time can be reduced by introducing, for example, voice recognition systems allowing doctors to dictate notes directly into electronic medical records. But is more time for the patient also safe for the doctor?
According to a study carried out in Europe, about 1/3 of european doctors think about changing their profession, and half of those experiencing burnout do not seek help, fearing stigmatization. One of the risk factors is emotional exhaustion. Empowered patients expect more and more attention. Doctors have to analyze more and more information. The pressure on productivity is increasing.
On the one side, computers are like a barrier between the doctor and the patient. On the other side, they are also a comfort zone, allowing the doctor to keep a healthy distance and make a break during intensive shifts with many patients. We have to think about it “how close (to the patient) is too close” at doctors’ and nurses’ work.
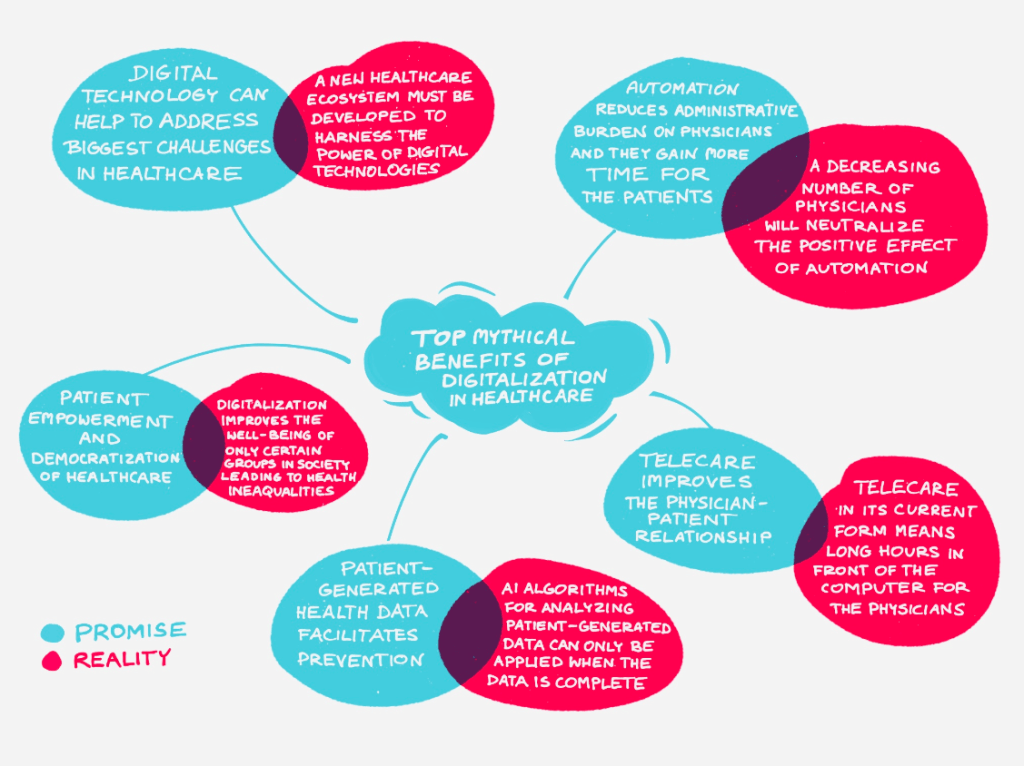
Myth #3. Patients and doctors want telecare
Telecare improves access to care. You do not have to waste time commuting. Your doctor becomes available even in the evening or at night. All you need is Internet access and a smartphone. Many tests – like ECG, blood pressure, blood oxygen – can be performed at home using a smartwatch. The results can then be transmitted to the doctor for a remote diagnosis. Health is now at your fingertips.
But what about doctors? Do they want such care? Does an 8-hour work shift in front of a computer gives them the same satisfaction as interacting with a patient in the doctor’s office?
In many cases, this is not the care model they expected when choosing a medical university. During the COVID-19, telemedicine has quickly gained momentum. It has undoubtedly its advantages. However, when thinking about the benefits of new digital care, it is essential to consider both patients’ and doctors’ needs.
Besides, digitization requires doctors to analyze gigabytes of data stored in electronic patient records, including data delivered by the patient. It will still take many years before the AI-systems will take over this task. Until then, the doctor will have to spend more time looking for relevant data in the overloaded electronic medical records.
Myth #4. Greater patient involvement
Digitalization is a key to the democratization of healthcare, claims Eric Topol in the book “The Patient Will See You Now.” According to Topol, easier access to information means that patients are better informed, and medical knowledge is no longer reserved exclusively for doctors. Emerging technologies, such as smartwatches measuring health parameters and fitness apps, provide better insights into health, making it easier to make decisions about one’s well-being. Each of us becomes a conscious architect of our own health.
However, this has nothing to do with democratization. As for now, only a small fraction of people can benefit from what technologies offer, and new digital inequalities arise. Besides, the degree of involvement in taking care of one’s own health (an active or passive role) depends on many determinants: living environment, education, economic and social status, housing, culture. In other words: Giving a smart fitness band to citizens in financial hardship will not improve their health overnight.
What can we do about it?
Instead of using digital technologies’ real powers, we focus on utopian dreams about digital as a solution for all problems. Undoubtedly, healthcare can become more efficient, patient-oriented, precise, and individualized by implementing digital solutions only if the healthcare economy will be upgraded. Adding technology to the old “status-quo” will make the existing systems similarly inefficient but more expensive.
We can’t just add technologies to what we have now, expecting a substantial change. The movie from Apple and Microsoft is a result of just this kind of old technology-driven approach. Even online consultations in the present form are only digitalized in-office visits. They do not offer extra value and therefore are often seen as a worse substitute.
We need a paradigm change towards a new model of healthcare in a digital era.

Did you like the article?
This website is free of commercials. Please support free journalism and aboutDigitalHealth.com (€1+). It only takes a minute. Thank you!
€1.00
What a great article ! Playing devils advocate is tricky but this is done in such a balanced way .. presenting the problems with a suggested solution . Much too often we get carried away with the promises of digital health technology without acknowledging the real, on the ground difficulties faced by end users . Kudos to an enjoyable read 🙂
LikeLiked by 1 person