With changing health care reimbursement models, growing consumer demand, and advances in digital technologies, virtual care is a must-have for health systems. But how can hospitals and health systems gain physician buy-in? It might be easier than you think. Deloitte presents the results of 2018 Survey of US Physicians.
Source: Deloitte
Virtual care programs will likely become increasingly important to health systems that want to retain and attract customers—consumers, employers, and health insurers—who will likely demand more connected, coordinated, and convenient care. No longer a futuristic idea, virtual care has the potential to transform care delivery by meeting consumers where they are, through multiple channels.
The Deloitte 2018 Surveys of US Health Care Consumers and Physicians have found that consumers and physicians agree on the benefits of virtual care. Consumers point to convenience and access (64 percent) as important benefits. Physicians agree that virtual care supports the goals of patient-centricity. The top three benefits from physicians’ perspective are:
- Improved patient access to care (66 percent)
- Improved patient satisfaction (52 percent)
- Staying connected with patients and their caregivers (45 percent)

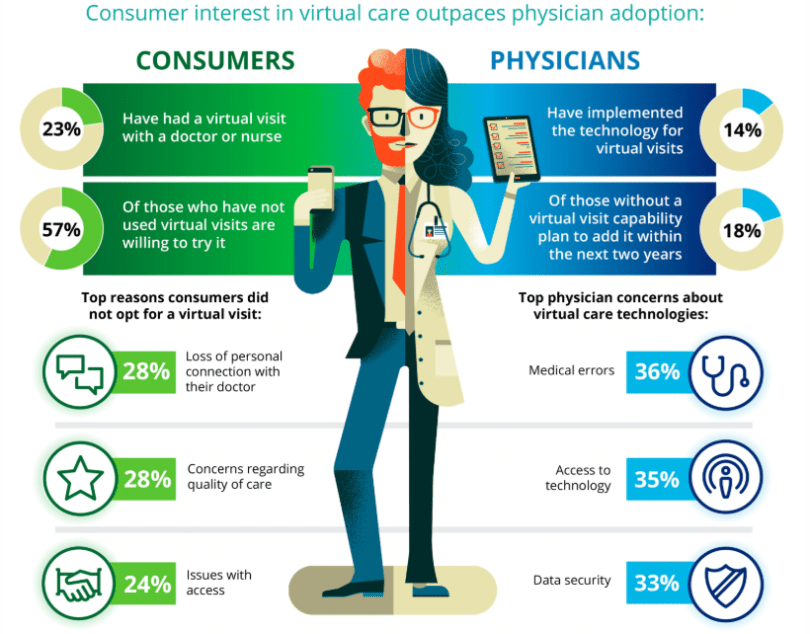
However, despite seeing eye to eye on the benefits, consumers and physicians diverge in their intent to use virtual care. While only 23 percent of consumers have had video visits, 57 percent of those who have not used them yet are willing to try them in the future. The interest from physicians is much lower: 14 percent of physicians have video visit capability today and only 18 percent of the rest plan to add this capability in the next year or two.

What explains physicians’ low interest in virtual care technologies?
Lack of reimbursement, complex licensing requirements, and the high cost of the technologies have contributed to slow adoption. Reliability and security are also issues: We found that physicians are concerned about medical errors (36 percent) and data security and privacy (33 percent).
That said, the market increasingly supports new care models. Our view is that with the changing reimbursement models, growing consumer demand, and advances in digital technologies, virtual care is a must-have for health systems, and they will now need to help physicians adopt virtual care capabilities.
Virtual care typically requires an enterprise approach as part of organizations’ overall strategy. Answers to several questions can help organizations articulate their goals and priorities and think through potential challenges:
- What issues can virtual care programs solve that traditional operations cannot?
- What value do these programs generate and how do they affect existing brick-and-mortar revenue?
- What assets are needed?
- Which patient populations should be targeted?
- What are traditional and nontraditional competitors doing around virtual health?
Health systems should act decisively to accelerate the adoption of virtual care, overcoming physicians’ reluctance. Despite the current low rates of both adoption and plans for adoption in our study results, answers to other survey questions suggest that gaining frontline physician buy-in may not be as hard as it appears. Physicians with experience of virtual care technologies tend to feel good about them: For each of the seven technologies available to them, large proportions of physicians (58–69 percent) expect to increase their use.
As organizations move from planning to execution, we offer a few tactical considerations in the following areas for helping physicians adopt virtual care:
- Workforce readiness and engagement
- Technology infrastructure and interoperability
- Operations and workflow integration
- Care model design
Click here to read the full summary.